The race to conquer COVID
A UC timeline from outbreak to vaccine
As the world turned the chapter on a new decade, a terrifying virus emerged that would quickly tear across the globe, taking an immeasurable toll on lives and livelihoods.
It also launched a historic mobilization of health care and science, leading to the delivery of a safe, effective vaccine in under a year and giving us new tools to fight future pandemics.
This is how the outbreak unfolded and how the University of California — and its vast health enterprise — played a role in the research, technology and patient care that is taking us from crisis to cure.
A killer arrives
In the last few hours of 2019, China alerts the World Health Organization that a mysterious, pneumonia-like illness has emerged in Wuhan. Within a few weeks, it has appeared on the West Coast.
As a cruise ship of infected passengers idles in the waters off California, UC hospitals admit and treat some of the earliest patients. Meanwhile, with scientists and public health officials working overtime to gain an understanding of the disease, UC marshals its leading experts to help the state prepare for the coming health tsunami. It also develops protocols to look for suspected cases, leading UC Davis Health to identify the first case of community transmission in the U.S.
I brought together experts to think about how to protect our hospitals, patients, health care workers and campuses. I asked our health center CEOs, ‘What will we do if 10 or 20 percent of our patients have COVID?’ This was what we had to prepare for. A pandemic was coming.
Dr. Carrie L. Byington
Infectious
disease expert,
executive vice president,
University of
California Health
-
Cluster of mysterious, pneumonia-like cases appears in Wuhan, China
-
Dr. Carrie L. Byington is only a few weeks into her post as executive vice president of University of California Health (UCH) when she learns about the cluster of cases of a contagious and deadly new virus halfway across the globe. A specialist in infectious diseases, Dr. Byington recognizes the potential threat. She begins gathering experts from across the UC system to advise on key areas of emergency response, preparing health systems, campus and employee operations for the possibility of an emerging pandemic.
-
First case of COVID in the U.S. diagnosed, in Snohomish, Washington
-
When a previously healthy woman is transferred to UC Davis Medical Center with a severe respiratory infection and tests negative for all common viruses, her doctors immediately suspect the novel coronavirus. But CDC guidance says that people who haven’t traveled to China or been in close contact with someone who has should not be considered to have the disease.
A UC-wide team of experts has been on the lookout for community spread and developed a protocol for identifying suspected cases. They press the CDC to test the patient, who does indeed test positive. She is treated with remdesivir as part of an early UC Davis clinical trial and ultimately recovers.
The positive diagnosis, however, is proof the virus is now circulating in the community. It transforms the way the CDC and the nation respond to the disease.
-
First US COVID fatality is reported, in a Washington nursing home
-
With the coronavirus barreling down on California, UC leaders call on Congress to pass legislation to combat the spread of COVID-19, support students and faculty transitioning to remote instruction and help researchers racing to develop vaccines as well as the health and medical professionals on the front lines treating the pandemic.
Throughout the pandemic, UC will continue advocating for the needs of the community and state. Ultimately, federal relief bills will provide more than $2.3 billion to help UC support the direct and indirect costs of responding to the pandemic.
-
With fewer than 500 CDC-issued test kits available to health providers across the country to diagnose the virus, the U.S. is already facing a dire testing shortage when a problem with a reagent renders many of the existing tests unusable. The University of California Health (UCH) joins labs across the country to petition the FDA to develop their own.
After the agency grants emergency use authorization of in-house testing, UC’s five medical centers quickly develop and ramp up capacity. UCH becomes one of the first academic health systems in the U.S. able to test for the novel disease.
California races to flatten the curve
As intensive care units in New York and elsewhere fill up with coronavirus patients, scientists and health officials launch an all-out effort to treat the sick and stop the virus from spiraling out of control.
California takes an aggressive stance on containment and is the first state to institute sweeping stay-at-home orders aimed at halting the pandemic’s spread. By mid-March, schools and non-essential businesses are shuttered. The era of social distancing has begun.

ICU nurse Stephanie Lichtwardt works 12-hour shifts and goes weeks without seeing her young son to care for COVID-19 patients at UC San Diego Medical Center. For many, she has become like second family.
Credit: Kyle Dykes/UC San Diego Health
-
As harrowing scenes from Italy and then New York City show capable health care systems being overwhelmed, UC moves into action to meet the governor’s call for expanding capacity. Command centers are established to keep running tabs on available beds, staff and equipment and to assess where patients can be transferred at any given moment.
UC hospitals are ultimately able to more than double their capacity to care for the critically ill.
-
Dr. Byington addresses the California assembly to share facts, urge action steps and lay out the challenges ahead. At the same time, the University of California Health Coordinating Committee — comprised of leading experts in epidemic and emergency response — is launched to guide UC campuses and health centers’ planning. The committee helps UC hospitals prepare for the incoming surge of patients and establish standards for allocating scarce resources, along with helping campuses develop guidelines for reducing transmission of the virus.
-
WHO declares COVID a global pandemic
-
To mitigate transmission of the novel coronavirus, campuses starting with UC Berkeley announce they are suspending in-person classes and moving to remote instruction for a period of at least two weeks. In just a few days, campuses close most public buildings, suspend on-campus research and order all non-essential employees to work remotely. Students who have a safe place to live and study are asked to vacate campus housing.
-
California issues statewide stay-at-home order
-
Nobel laureate-to-be Jennifer Doudna, the lab’s founder, shelves all existing research projects to focus exclusively on the coronavirus. Step one: stand up a diagnostics lab that can process 1,000 tests a day with results within 48 hours.
-
By seeking a potential cure from among dozens of drugs that have already been approved as safe for human use, the team hopes to cut years off the time it can take to develop a new therapy. By December one stands out: an anti-cancer drug that demonstrates promising results in helping some hospitalized patients recover.
-
UC’s three national labs — Lawrence Berkeley National Lab, Lawrence Livermore National Lab and Los Alamos National Lab — answer a call from the White House to harness the country’s most advanced computing power to speed discovery in the fight against COVID. Through the initiative, the labs contribute the power of their world-class supercomputing facilities to unravel the mysteries of the novel virus, from understanding its structure and identifying potential drug targets to predicting likely variants.
-
The antiviral medication becomes the first FDA-approved treatment for COVID-19 after clinical trials show it improves survival rates for patients with severe illness.
Altogether, UC health centers take part in more than 100 clinical trials testing new and existing drugs as therapies for use in treating COVID-19.
The science advances
As the death count grows, UC researchers race to understand how the virus operates and how it can be stopped, while UC medical staff step up to provide care for patients in the nation’s hardest-hit areas.
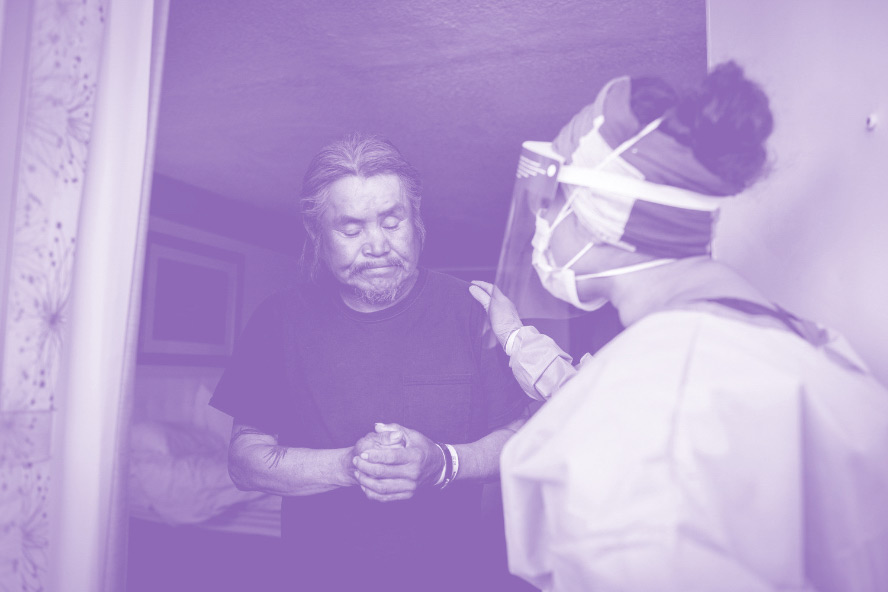
UCSF sends teams of doctors and nurses to fight COVID in the Navajo Nation.
Credit: UCSF
-
California and the CDC recommend use of cloth masks
-
UC’s Office of the President provides more than $2 million in micro-grants to jump-start new research initiatives. The effort enables a wide array of research projects — from a UC Riverside study on how vaping and nicotine impact COVID outcomes to a UC Santa Cruz effort to provide better supports to vulnerable communities — to gear up quickly and begin delivering results.
-
California experiences the first surge as 5,792 patients are hospitalized with the coronavirus
-
Along with fever, fatigue and shortness of breath, a UC San Diego study validates loss of smell and taste as important early signs of COVID-19 infection. The study finds people with those symptoms are 10 times more likely to have COVID-19 than any other illness, offering the first empirical evidence of the link.
-
At a time when local health departments are struggling to understand who has the disease and how widespread it is, the effort proves crucial to enabling communities across the state to set up testing programs for their residents. By mid-2021, along with serving hundreds of thousands of UCH patients, UC labs process almost 650,000 tests for public health departments, nursing homes and other health systems.
-
The influential study, by engineering professor De Kai, finds that communities can flatten the curve and safely resume normal activities by reaching 80 to 90 percent mask compliance. His computer simulation program called “masksim” lets users test the results for themselves.
-
Dozens of health professionals volunteer to provide critical care in the Navajo Nation of Arizona and Utah, an area with limited access to quality health care that has been devastated by the pandemic. Another team heads out to New York to assist in the unfolding crisis there.
-
At a time when few people without symptoms are able to get a COVID test, a UCSF initiative called Unidos in Salud tests 6,000 low-income, Latinx neighborhood residents and uncovers the community’s high rates of infection. The effort provides one of the first snapshots into how widely COVID is circulating, including among those without symptoms. The study also spotlights socioeconomic factors, including cramped living and working conditions, which are accelerating the spread and leading to disproportionately high infection rates among some groups.
-
Lawrence Berkeley National Lab scientists launch a machine learning tool to help scientists harness and make use of the exploding array of research into what the novel coronavirus is and how it operates. Called COVIDScholar, the free tool uses natural language processing techniques to scan and comb through thousands of research documents, and help draw insights and connections that may otherwise not be apparent.
-
Partnering with local health departments in each of California’s 58 counties, the campuses mount a massive training program to train and deploy 20,000 residents to serve as contact tracers across the state. The program engages city librarians, attorneys, medical students, retired public health officials and others as “disease detectives” who can track the spread of the virus and notify individuals who may have been exposed.
New tools emerge to battle the disease
As the pandemic ushers in a summer like no other, UC joins an unprecedented nationwide effort to find a coronavirus vaccine. By the end of the summer, UC is participating in all major vaccine trials, including those for Pfizer, Moderna and Johnson & Johnson. Hope grows that vaccines might be available by year’s end.
The university also continues to push development of new technologies that could play a breakthrough role in halting the virus, such as saliva testing and a nasal spray to prevent severe COVID infection.
It was the most intense feeling of relief that I had ever felt. It was this wave of hope. Then I got back to work, because it wasn’t done.
Stephen Hoge
President of Moderna and
UCSF alum, upon the
FDA’s announcement that
Moderna’s COVID vaccine was 100 percent effective in
preventing death.
-
California issues statewide mask mandate
-
The National Institutes of Health kick off nationwide clinical trials to test vaccines against the coronavirus. UC health centers are involved in virtually all the high impact trials, thanks to coordination and agreements established early in the pandemic.
A top UCH priority: Ensure that clinical trials include large numbers of people from diverse populations and socioeconomic groups. UC’s strong community partnerships and its use of pop-up clinics help enlist participants in hard-to-reach communities.
Shots start going into arms very quickly over the summer and fall; participants begin testing the Moderna vaccine at UC San Diego in July, while in August, UC Davis begins inoculating the first of 200 participants in Pfizer vaccine trials.
-
California’s second, more deadly surge sees more than 8,000 hospitalized and 150 deaths a day
-
A team of researchers engineers synthetic molecules that can be sprayed into the nose and mouth to prevent severe coronavirus infection. AeroNabs works by hijacking and disabling the machinery the virus uses to infect cells. It could ultimately offer a valuable extra layer of protection against COVID, even in a largely vaccinated population, and provide an easy-to-distribute way to fight COVID in countries without sufficient supply of the vaccine.
-
With most colleges and universities operating under remote instruction, almost 6,000 undergraduate students start moving onto UC San Diego’s campus over a 10-day period as part of its Return to Learn effort. The comprehensive COVID-19 testing and monitoring program ranges from testing wastewater for outbreaks to offering free COVID tests in the vending machines.
The measures allow the campus to keep infections extremely low, at a fraction of the rate of the county as a whole. Many universities and schools will draw on the effort to establish their own safe return practices.
-
The FDA grants emergency authorization to SwabSeq, a technology by UCLA researchers and a UCLA startup that enables providers to test thousands of coronavirus samples simultaneously and return results with 24-48 hours.
With widely used testing practices requiring days and sometimes weeks to get results, the technology — ultimately adopted at UC campuses and dozens of other institutions — lays the groundwork for much more widespread, faster results testing.
-
The clinic is one of the first to help those who suffer lingering symptoms long after acute illness has passed. Along with providing care, UC also provides research to further understand the breadth and depth of the problem; it finds that 1 in 4 people infected by COVID-19 have lingering symptoms.
-
Using an app developed by Apple and Google, the program anonymously alerts users if they’ve been in contact with someone who tests positive for COVID. UC San Diego Health partners with the state to roll out CA Notify and enroll millions of Californians.
In the darkest days, hope arrives
The darkest days of the year see the U.S. case and death counts soar to their highest proportions. And yet, hope appears as a vaccine — the most rapidly developed in human history — is authorized for use.
UC health centers administer some of the first doses, kicking off a journey to get the vaccine into the arms of millions of people across the U.S. Advances in testing, diagnosis and treatment are also part of a path that it is hoped will ultimately lead to the end of the disease.
I took care of the first [patient] to get community acquired COVID-19. Since then, there has been a lot of death. I was and am so tired. But with the vaccine, there came a lightness. So side effects? Arm soreness and hope.
Janelle Vu Pugashetti, M.D.
Pulmonary
and critical care fellow, UC Davis
-
With cases surging and ICUs nearing capacity, California enacts stay-at-home order through the holiday season
-
As people brace for a lonely and frightening holiday season, UC health providers work tirelessly to combat the worst surge California has experienced. But thanks to emergency planning UCH adopted early on in the crisis, the hospitals are able to respond without running out of ventilators, staff or ICU beds.
-
FDA grants Pfizer vaccine emergency use authorization
-
UC hospitals commit to equitable distribution of the vaccine for anyone who works in patient care, regardless of seniority or job status. At UCSF, the first person to receive the vaccine is senior custodian William Wyatt, a 30-year employee who cleans patients’ rooms.
-
The Moderna vaccine is approved for emergency use
-
Fearing a shortage of ICU beds, UC Irvine Medical Center puts up field tents in a parking lot to provide an extra 50 beds. The unit provides emergency room and inpatient services, freeing up more beds inside the hospital to care for COVID patients in intensive care.
The march toward immunity begins
With record-breaking numbers of hospitalized patients and troubling new variants emerging, the race to get shots into arms is on. A big part of UC’s role: inoculate vulnerable and hard-to-reach populations.
Cases recede as vaccine eligibility slowly expands, starting with older residents. Grandparents hug grandchildren. Businesses reopen. As a long locked-down state slowly emerges from hibernation, a new sense of promise takes hold.
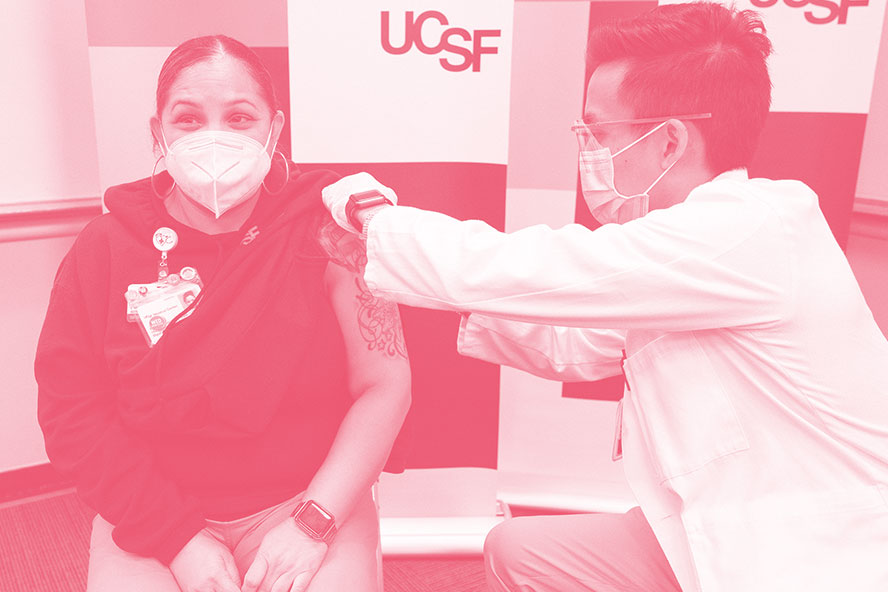
Reina Lopez, a patient support assistant in UCSF Hospitality Services, receives a COVID-19 shot on the first day UCSF distributes the vaccines to its frontline workers.
Credit: UCSF, Susan Merrell
-
California hospitals see an all-time high of almost 29,000 patients
-
Two weeks after the Knight Lab at UC San Diego Health discovers that the so-called U.K. variant — a more contagious and deadly strain of COVID — has appeared in California, UC San Francisco doctors discover a brand new strain has emerged in the state, making up roughly a quarter of samples tested. The new strain, dubbed the California variant, will quickly become dominant in the state.
-
In partnership with county and city officials as well as the San Diego Padres, who offer to share their home at PetCo stadium, UC San Diego Health accelerates early vaccine distribution, taking only six days to stand up one of the first mass vaccination sites in California.
Administering 5,000 shots daily to frontline health care workers and residents over 65, the site delivers more than 200,000 doses before closing up shop at the end of March, when the stadium reopens for Major League Baseball. The project provides a blueprint (covered in the Journal of the American Medical Association) to help others create mass vaccination sites.
-
Biotechnology firm ConserV Bioscience is evaluating a platform developed by the UC-run national lab as a potential delivery system for the firm’s mRNA technology, with the goal to develop a universal coronavirus vaccine.
If effective, the vaccine would prevent infection not only from new COVID variants, but even viruses that don’t exist yet. The technology targets the immune response to parts of proteins on the virus that, unlike the spike protein, don’t mutate. If animal trials are successful, human trials could begin as early as the beginning of 2022.
-
After a year-long effort by researchers at UCSF’s Quantitative Biosciences Institute to find a potential treatment for COVID within existing drugs, researchers hit the jackpot with an anti-cancer treatment that shows potential to kill the coronavirus and is 30 times more potent than remdesivir in helping severely ill patients survive.
-
In an effort hailed as one of the most ambitious in the nation, UC Davis devises a plan to use its expertise and resources to keep the entire community safe from the coronavirus.
Through the plan, the university provides twice-weekly testing, masks, free quarantine housing and vaccines to every resident of the town of Davis. It also enlists an army of students as contact tracers and monitors wastewater to halt outbreaks of the disease.
-
Through community partnerships, UC establishes programs directly targeted to Black and Latinx residents, as well as vulnerable and non-English speaking residents across the state.
In early February, UCH and Mercy medical center set up a pop-up vaccination clinic to vaccinate up to 750 Central Valley residents over a multiday event.
Meanwhile, building on earlier programs to test underserved Bay Area communities, UCSF’s COVID Community Health Initiative sets up vaccine sites and pop-up clinics to inoculate thousands of unhoused, undocumented, and low-income people, as well as Black and Latinx residents across the Bay Area.
The program also taps physicians fluent in other languages to speak at community and union meetings, reaching more than 35,000 non-English speakers with information on how and why to get the vaccine.
-
Hundreds of staff, students and faculty donate their time to deliver vaccines to people across the state. Among them, UC President Michael V. Drake, M.D., returns to his roots as a medical provider to deliver injections at a community clinic in San Francisco’s Mission District.
California reopens
By spring, millions of Californians have lined up to get inoculations. Cases and hospitalizations plummet as immunizations climb.
After more than a year of grief and loss, joy erupts as friends and families reunite, people make travel plans, communities join in July 4th celebrations and students prepare to return to schools and campuses.
We will forever be shaped by the events of the past year — and by the hard work of so many members of the University of California community who came together to confront this global crisis. As the world works to put this crisis behind us, I know UC will continue to meet the moment with creativity, generosity and resilience.
Michael V. Drake, M.D.
UC
President
-
The COVID-19 vaccine becomes available to all California residents 16 and older
-
Racing against the spread of new and more deadly variants, teams from UC health centers deliver a milestone 1 million vaccine doses. At stadiums, UC health centers, community clinics and mobile vans, providers have worked tirelessly to inoculate Californians, helping the state achieve one of the highest vaccination rates in the nation.
-
UC’s five medical centers are part of a UCLA-led coalition that is working with the National Institutes of Health to test vaccine outreach and education strategies, especially among Black, Latinx and Indigenous populations that have historical reasons for mistrust of the medical community. The alliance, called STOP COVID-19 CA, produces research to inform vaccine campaigns across California and the U.S.
-
FDA clears use of vaccine for 12- to 16-year-olds
-
As the drive to vaccinate Californians turns to more localized efforts, UC San Diego Health administers the last of injections delivered at its RIMAC Arena vaccine supercenter. The first health center in the state to open a mass vaccine site, it will now shift its focus to mobile clinics and pop-up sites in the communities where people work and live.
-
California reopens, drops most pandemic-era restrictions
-
Biochemistry professor Philip Felgner, director of UC Irvine’s Center for Vaccine Research and Development, is among seven scientists honored by the Spanish government for pioneering the research that led to the development of COVID vaccines.
More than 30 years ago, Felgner developed a means of delivering DNA to cells known as lipofection technology. Felgner’s findings ultimately led to the development of DNA vaccines, which paved the way for the mRNA technology used by Pfizer and Moderna in their development of a COVID vaccine.
-
Scientists with the UC Irvine Health Gavin Herbert Eye Institute have designed a promising vaccine prototype aimed at preventing serious infections by all coronavirus strains and variants, not just the ones that cause COVID-19. The team plans to begin human trials of the vaccine in early 2022.
If all goes well, according to lead researcher Lbachir BenMohamed, a pan-coronavirus vaccine could be available by the end of 2023.
Where we go from here
In the year and a half since COVID-19 made its deadly appearance, we have developed tools to fight back. The toll in lives and livelihoods has been enormous, and the virus continues to rage in many countries around the world. At home, there is still work to be done to reach vaccine-hesitant populations and keep the coronavirus permanently at bay.
UC will continue to push science forward to put this crisis behind us for good — and help us head off a future pandemic.
Will they work for youth? Will we need boosters? University of California Health is leading clinical trials to find out, such as one at UC Davis to test how well the vaccine responds to variants. UCSF is leading a study on how sleep and stress affect the vaccine’s efficacy. Meanwhile, UC and national lab researchers are looking into easier ways to deliver the vaccine, from wearable skin patches, to probiotic vaccines that could be taken as a food supplement.
Two cancer drugs separately identified by researchers at UCSF and UCLA hold promise in helping sick patients recover. There may be more such discoveries on the horizon.
Studies like one by researchers at UC Davis’s clinic for long-haul COVID are looking to understand more about the lingering nature of some COVID cases, as scientists across UC develop approaches to relieve its symptoms.
UC is building on community partnerships that it established during the pandemic to build trust and bring vaccines to thousands of unhoused people and underserved communities around the state.
UC is working to develop treatments that are easier to store and transport than the current vaccines. A technology like AeroNabs, that can immediately lessen viral load through an inhaler-like delivery, could help fight the virus in places that are harder to reach.
From starting trials on a vaccine against all coronaviruses to searching for viruses most likely to spill over into human populations, UC researchers are already hard at work on the technology and tools to prevent the next pandemic.
UC Irvine and Lawrence Livermore National Labs are among those pursuing development of universal coronavirus vaccines. Clinical trials could start as soon as early 2022.
At UC Davis, the PREEMPT program is trying to identify and contain high-risk pathogens before they leave their animal sources, while at the UC Irvine Center for Virus Research, scientists are looking at strategies to create vaccines for diseases that don’t yet exist.